Abstract
Oral squamous cell carcinomas (OSCC) signs and symptoms may be first identified by dental hygienists during routine extra and intra-oral examinations. A comprehensive extra-oral and intra-oral examination during regular dental hygiene assessment is paramount to identifying oral potentially malignant disorders (OPMD) and cancerous lesions for timely referral and treatment. Integrating a systematic list of questions during the medical and dental assessment along with careful visual and tactile examinations is critical to identifying OPMDs and cancerous lesions. Understanding the relationship between oropharyngeal squamous cell carcinomas (OPSCC) and Human Papilloma Virus (HPV) and how vaccination can prevent HPV-related OPSCC is critical to providing evidence-based recommendations and care. The purpose of this report is to provide an update on current epidemiological trends of OSCC and OPSCC rates in the United States (US) and provide the latest evidence on what dental hygienists must know to improve health outcomes and mitigate the consequences of undiagnosed cancer. This report considers enduring challenges with the annual rise in OPSCC rates and the public health burden of HPV-related cancers in the US. Emphasis on regular, quality continuing education about OSCC and OPSCC is emphasized along with recommendations for evidence-based training.
- Oral squamous cell carcinoma
- oropharyngeal squamous cell carcinoma
- oral potentially malignant disorders
- human papillomavirus
- extra oral examination
- intraoral examination
- HPV vaccine
INTRODUCTION
Cancer surveillance remains an essential component of health care delivery and is critical to dental hygiene practice. Cancer remains a leading cause of mortality both globally and in the United States (US), with oral and oropharyngeal cancer rates remaining persistently high.1 The American Cancer Society estimates 58,450 new cases and over 12,230 deaths related to oral cavity and oropharyngeal cancers in 2024.2 Moreover, the incidence of oral squamous cell carcinoma (OSCC) and oropharyngeal squamous cell carcinomas (OPSCC) continues to rise at approximately 1% per year, with mortality rates for human papillomavirus (HPV)-associated OPSCC increasing at approximately 2% per year.2,3
Dental hygienists are often the first healthcare providers to identify risk factors, along with signs and symptoms related to head and neck cancers in their patients. Detecting cancer in the earliest stages is critical to favorable treatment outcomes, improving quality of life, and preventing loss of life. This short report provides a summary of the risk factors, signs, and symptoms of OPSCCs and OSCCs along with the role of the oral health care professional in patient referral and supportive care.
Oral Squamous Cell Carcinoma
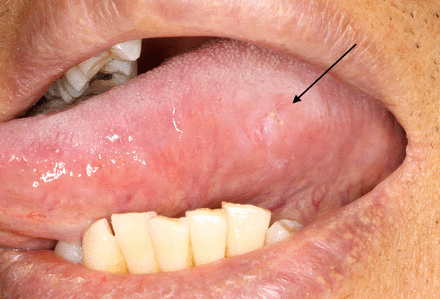
Oral squamous cell carcinoma (OSCC) is the most common type of cancer found within the oral cavity. Some OSCCs may arise from oral potentially malignant disorders (OPMDs). The oral cavity comprises multiple sites covered with oral mucosal epithelium including the labial and buccal mucosa, the anterior two-thirds of the tongue, retromolar trigones, floor of the mouth, gingiva, and palate. Malignant lesions in the early stages are often asymptomatic, whereas lesions in more advanced stages may present with pain and bleeding. Oral squamous cell carcinoma may present in the oral cavity as a non-healing ulcer, white or red plaques or mass. Abnormalities associated with an OSCC may be detected upon careful visual and tactile examination and should also include relevant information obtained from a thorough patient interview. Figure 1 shows an early-stage squamous cell carcinoma on the left lateral border of the tongue.
Early squamous cell carcinoma, left tongue
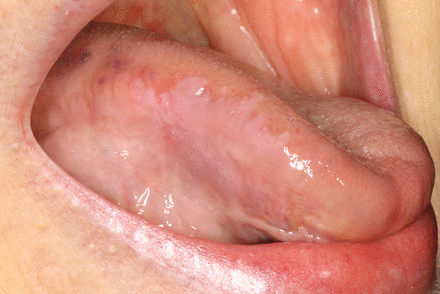
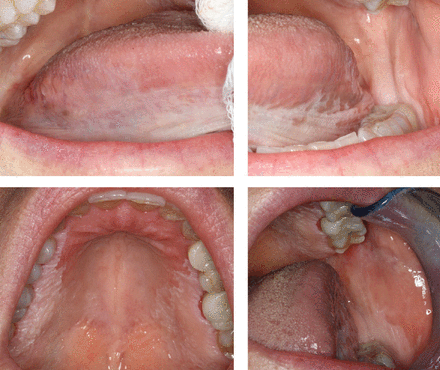
Oral potentially malignant disorders are oral lesions associated with an increased risk of progressing to an OSCC.4 Types of OPMD lesions include leukoplakia, erythroplakia, lichen planus and submucous fibrosis; leukoplakia is the most common OPMD in the US. The estimated global prevalence of oral leukoplakia is 1.39% and typically presents as a white plaque with well-defined margins (homogenous localized leukoplakia). Localized leukoplakia presenting on the right lateral border of the tongue is shown in Figure 2. Common risk factors for oral leukoplakia include age (> 50 years old), male sex, and history of tobacco use.4–6 However, proliferative (verrucous) leukoplakia (multi-site leukoplakia or one large single-site leukoplakia) is more common amongst females with no known risk factors.7 Proliferative, multi-site leukoplakia is shown in Figure 3. Clinical manifestations and malignant transformations of common OPMDs are shown in Table I.
Localized leukoplakia, right tongue
Oral proliferative leukoplakia, multiple sites.
Patients with OPMD should be referred to a dental specialist (e.g. e.g. oral medicine specialist, oral pathologist, or oral surgeon) for further evaluation and management. Biopsy for definitive diagnosis and surgical excision remains the standard approach to treating patients with localized oral leukoplakia even though the 5-year recurrence rate is common (49%).8 Other treatment options include laser ablation, a watch-and-wait approach with surveillance biopsies, and topical therapy, although some of these modalities have also been associated with recurrence.8
Early detection of OSCC and OPMDs includes a detailed patient history and assessment of risk factors including type and frequency of tobacco and tobacco products, use and frequency of alcohol products, betel quid and areca nut use, UV light exposure (for lip cancers; i.e., excessive sun exposure and tanning beds), genetic syndromes (such as Fanconi anemia and Dyskeratosis congenita), a proinflammatory diet, low socioeconomic status, and previous or familial history of oral cancer.9–15
In the absence of any validated OSCC and OPMD screening tools, a thorough extra and intraoral examination, along with a detailed patient intake remain the standard of care and are vital to timely to early detection and referral for a definitive diagnosis and treatment.11 Recent advances in the molecular detection of cancer, particularly the use of liquid biopsy, hold promise for a non-invasive early diagnosis and risk prediction, however, the current gold standard for diagnosing an OSCC or OPMD remains the incisional biopsy.8,16
Oropharyngeal Squamous Cell Carcinoma
Oropharyngeal squamous cell carcinoma can manifest in the oropharynx, which is comprised of the palatine and lingual tonsils, the base of the tongue, soft palate, and posterior pharynx. According to data from the Centers for Disease Control, approximately 20,800 of the OPSCCs reported annually in the US are associated with persistent high-risk HPV infection.17 The incidence of HPV-positive cancers in the US has steadily increased over the past three decades, with a significant rise in new cases of HPV-positive OPSCC now surpassing the incidence of HPV-positive cerv¬ical cancer.2,18,19 Risk factors attributed to OPSCC include tobacco use and heavy alcohol consumption, increased age (>45 years), persistent HPV (16, or 18) infections of the oropharynx, areca nut (betel quid), immunodeficiency and diet.20,21 The risk of developing an HPV-positive OPSCC is higher for individuals who have been exposed to HPV, particularly HPV 16 and HPV 18.19,22 Persistent HPV infection is associated with a high number of lifetime sexual partners and the prevalence is higher among men than women, as well as in individuals who smoke tobacco.23
Oropharyngeal squamous cell carcinoma may not be seen in the unaided visual examination, as most of the oropharynx is not visible from the oral cavity. This underscores the importance of a comprehensive patient history and extra oral examination with lymph node palpation. The dental screening examination for OPSCC requires a thorough patient interview along with visual and tactile examinations of the head and neck region. During the external examination and lymph node palpation, the oral health care provider should inquire about any prolonged difficulty in swallowing (dysphagia), unilateral ear pain (otalgia), sore throat, difficulty swallowing (dysphagia) and/or enlargement (swelling/lump) in the throat or neck. A sore tongue or swelling/lump on tongue, changes to voice have also been associated with OPSCC.24 Any positive finding(s) should be documented, reviewed with the patient, followed by referral to a specialist for further evaluation.
A timely and appropriate referral to a head and neck specialist for further examination is vital to proper diagnosis. A list of potential specialists should be readily available for a seamless referral. Providers such as an ear, nose, and throat (ENT) physician, have expertise in OPSCC and will order the appropriate examinations (i.e., indirect, or direct pharyngoscopy or laryngoscopy) and tests (biopsy) for a definitive diagnosis. A referral to the patient’s general practitioner may be required first depending upon insurance coverage and referral guidelines. The oral health care provider should follow up on the patient’s referral progress and offer guidance as needed for navigating the proper channels for a timely diagnosis.
Post-Referral Follow-up and Oral Care
Cancer treatment for OSCC and OPSCC involves a multidisciplinary team of providers, including the dentist and dental hygienist. Dental providers can provide essential care and support before, during and following treatment that usually involves a multidisciplinary approach including surgery, radiation, and chemotherapy. Chronic post-treatment side effects may include difficulties with mastication, loss of teeth, partial or comprehensive loss of salivary gland function, increased risk of dental caries and periodontal disease, osteoradionecrosis, loss of taste, orofacial neuropathies, difficulty with speech and swallowing, trismus, and ongoing challenges with oral hygiene.25–27 Dental providers should communicate regularly with the oncology team to provide the best possible outcomes during treatment and facilitate a care plan to support the patient’s long-term oral health.
Head and Neck Examination
Screening for head and neck cancers is a standard of oral health care delivery and should be part of the extra and intraoral head and neck examination. A comprehensive examination includes a careful review of a patient’s medical, social, and dental histories, followed by a visual and tactile examination both extra and intraorally to screen for abnormalities and pathologies including oral potentially malignant disorders (OPMDs) and potential OSCC and OPSCC.11 Early detection of OPMD and oral cancer along with an appropriate referral are essential measures for optimal, timely, and potentially life-saving treatment. It is critical to develop a consistent protocol for the visual and tactile head and neck examination.28, 29 The components of the head and neck examination are shown in Table II.
HPV Vaccination as Cancer Prevention
Dentists and dental hygienists should routinely discuss the importance of HPV vaccination with their patients, as research demonstrates an HPV vaccination recommendation from a health care provider is associated with a 10.1 - fold increase in HPV vaccine uptake.30 Dentists and dental hygienists should avail themselves to the wide range of current, evidence-based resources on HPV vaccination as cancer prevention. The American Cancer Society, American Dental Hygienists’ Association, and the Centers for Disease Control and Prevention are just a few of the many credible organizations that offer HPV cancer prevention training and/or materials for providers and their patients. Continuing education on HPV will support professional understanding and facilitate effective conversations and recommendations for the vaccine. Additional measures for improving HPV vaccination educational efforts include adding a question about HPV vaccination status in the medical history and engaging in motivational interviewing during patient education. Having resources available to share following patient education such as QR codes and pamphlets about the benefits of the vaccine are helpful reminders to vaccinate.
The American Cancer Society and the American Academy of Pediatrics recommend routine HPV vaccination for children beginning at age 9.30 Initiating HPV immunization at age 9 increases the likelihood of a better immune response and offers a longer window of time to receive the second completion dose, ensuring the best possible protection before the first HPV exposure.31,32 As of 2022, vaccine coverage among US adolescents ages 13-17 years was 62.9%, and well below the national target aim of vaccinating 80% of US adolescents.33 Oral health care providers are well positioned to relay the importance of HPV cancer prevention to their patients and can serve both indirectly and directly in improving HPV vaccination rates.34 The COVID-19 (2019) and H1N1 (2009) pandemics led to the passage of legislation authorizing dentists and dental hygienists to administer vaccines in many US states, including the HPV vaccine.35–37
Oral health care providers have the potential to play a pivotal role in preventing OPSCC by increasing access to HPV vaccines, and providing the education and screening to reduce the incidence and morbidity associated with HPV-OPSCCs.
CONCLUSION
Oral health care providers are essential to the early detection and/or prevention of OSCC and OPSCC. Routine head and neck examinations as part of the screening process, along with patient education on risk reduction strategies, including the promotion of HPV vaccination, can have a positive impact on the health outcomes related to OSCC and OPSCC. Dental care providers should regularly update their knowledge and skills regarding head and neck cancer screening strategies, HPV vaccination and motivational interviewing techniques. Seeking evidence-based resources from credible organizations is critical to obtaining timely, accurate information about cancer detection and prevention.
DISCLOSURES
Alessandro Villa has received research support from Merk phamaceuticals.
Footnotes
NDHRA priority area, Professional development: Education (evaluation).
- Received March 15, 2024.
- Accepted March 29, 2024.
- Copyright © 2024 The American Dental Hygienists’ Association
This article is open access and may not be copied, distributed or modified without written permission from the American Dental Hygienists’ Association.